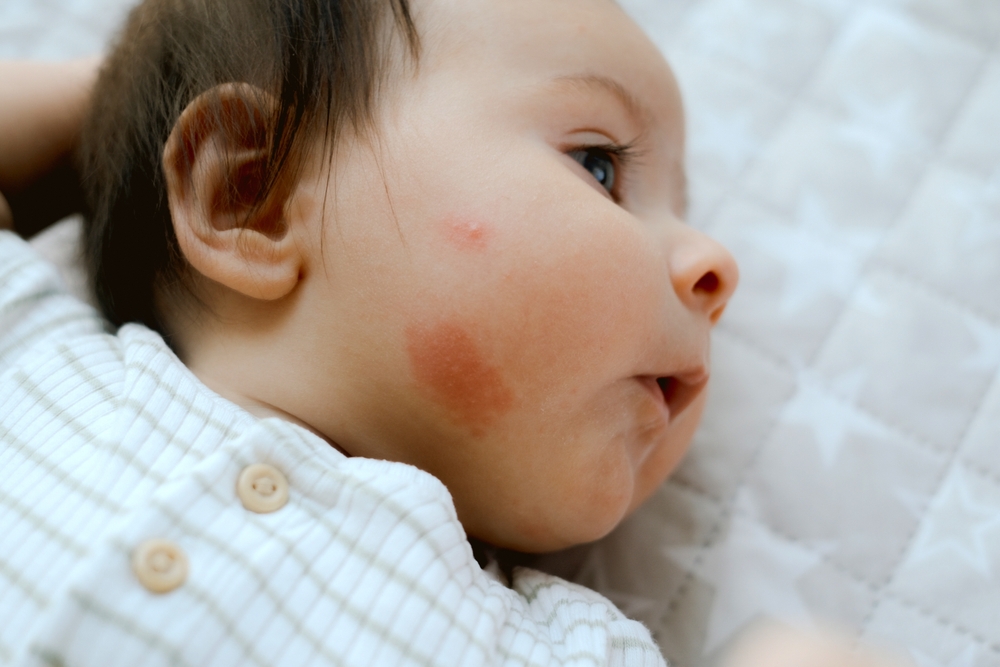
Discovering a red, raised mark on your newborn’s skin can trigger immediate concern. Vascular lesions affect many infants, making them one of the most common pediatric conditions parents encounter. While these blood vessel abnormalities can appear alarming, most are benign and manageable with proper medical evaluation.
Understanding the difference between vascular tumors like infantile hemangioma and vascular malformations such as port wine stain helps parents make informed decisions about their child’s care. The key is knowing when these marks require immediate attention and when watchful waiting is appropriate.
Breathe: Here’s What You Really Need to Focus On
- Most vascular lesions are benign conditions that don’t threaten your child’s long-term health or development.
- Accurate diagnosis matters because vascular tumors and vascular malformations require completely different treatment approaches.
- Location determines urgency more than size; lesions near the eyes, airways, or vital structures require prompt specialist evaluation.
- Modern treatments, including beta-blocker therapy and laser treatment, offer excellent outcomes for most cases.
- Early intervention prevents complications, though not all lesions require immediate treatment.
What Every Parent Needs to Know Right Now
Breaking down the confusion around vascular lesions starts with understanding the two main categories. Most parents have never heard these terms before their child’s diagnosis, but clear distinctions help you understand what you’re dealing with.
Vascular Tumors (Hemangiomas): These grow rapidly in the first year, then fade naturally over 5-10 years. Think of them as temporary visitors that usually leave on their own. The strawberry hemangioma’s appearance often causes alarm, but its predictable pattern offers reassurance.
Vascular Malformations (Port Wine Stains): Present at birth, these are permanent structural abnormalities of blood vessels. While lifelong, they’re manageable with proper treatment. Capillary vascular malformations and venous malformations fall into this category.
Tumors represent a contemporary cell-growth problem. Vascular malformations indicate a “plumbing problem” that’s permanent. This distinction determines if your child needs treatment now or can wait, directly affecting long-term care planning and family expectations.
According to the Children’s Hospital, understanding these categories helps physicians develop appropriate treatment plans based on each lesion’s specific characteristics and growth patterns.
The 5 Warning Signs That Mean “Call the Doctor TODAY”
Most lesions don’t need emergency care. But these five signs mean immediate specialist evaluation is necessary.
1. Breathing Problems
Lesions in the “beard area” of the face may affect the airway. Listen for noisy breathing, stridor, or difficulty feeding. Airway compromise can develop quickly in infants, making this the most urgent concern for any facial vascular lesions.
2. Vision Concerns
Lesions near or covering the eye require urgent attention. Watch for a droopy eyelid, an eye that doesn’t open fully, or your child favoring one eye. The first six months represent a critical window for vision development that can’t be recovered later.
3. Rapid Growth
A lesion that doubles in size within days or weeks warrants evaluation. This is especially concerning if near vital structures. Rapid expansion may indicate the need for immediate medication to prevent complications.
4. Bleeding or Open Wounds
Ulceration means breaks in the skin over the lesion. Signs of infection include warmth, pus, or spreading redness. These open wounds can be very painful for your baby and significantly increase the risk.
5. Feeding Difficulties
Lesions affecting the mouth, tongue, or throat can interfere with eating. If your baby struggles to eat or shows poor weight gain, this may indicate an underlying issue requiring a comprehensive evaluation by pediatric specialists.
When Your Baby Has a Hemangioma: What happens next?
Infantile hemangioma represents the most common vascular tumor in childhood. That scary red bump probably appeared around 2-4 weeks of age, started small, then seemed to explode in size. This is completely normal hemangioma behavior that follows predictable patterns.
Growth Phase (0-12 months): This is the scary part where it grows quickly, with peak growth usually by 3-5 months. Yes, it’s alarming, but it’s expected and doesn’t necessarily mean treatment is needed.
Plateau Phase (1-2 years): Growth stops, and the lesion just sits there. Many parents think it’s permanent at this stage, but this is just a pause before shrinking begins.
Shrinking Phase (2-10 years): Gradual fading occurs as the benign tumors naturally involute. Many show major improvement by age 5, though complete resolution can take longer.
Location determines treatment urgency more than size. Facial “beard distribution” lesions may affect the airways, while eye-area hemangiomas may cause vision problems requiring specialist evaluation. Diaper area lesions ulcerate more easily due to friction.
Propranolol revolutionized hemangioma care with high success rates when started before 5 months. This twice-daily liquid medicine shrinks blood vessels and stops growth, though it requires cardiac screening first.
Side effects, such as low blood sugar, are rare and monitored. Only problematic hemangiomas that affect function need medication—small surface lesions can be treated with topical Timolol maleate gel instead.
According to research published by the NIH, early intervention with beta-blocker therapy has dramatically improved outcomes for children with complicated hemangiomas.
Port Wine Stains and Permanent Vascular Marks: The Truth About “Birthmarks”
Unlike hemangiomas, these don’t go away on their own. Present at birth rather than appearing later, they grow proportionally with your child throughout life. The good news is that treatment technology has improved dramatically, with laser therapy offering excellent results.
The better news? Early treatment works better than waiting for your child to get older.
Port wine stains darken from pink to purple over the years without treatment. They can develop raised bumps and nodules in adulthood if left untreated. The skin thickens over time, making treatment more challenging. Laser therapy is most effective for thin, light-colored stains, which is why treating in infancy or early childhood yields better results than waiting.
Pulsed Dye Laser: This gold standard for treating capillaries (port-wine stains) targets blood vessels while protecting surrounding skin. Treatment requires multiple sessions spaced 6-8 weeks apart, with each session gradually lightening the mark.
Sclerotherapy: For deeper malformations, including venous and lymphatic malformations, doctors inject a sclerosing agent to shrink abnormal vessels. Pediatric interventional radiologists perform these procedures with specialized imaging guidance.
Combined Approach: Some complex vascular anomalies need both laser treatment and medication or surgical intervention for optimal results.
What “success” really means requires realistic expectations. Complete clearance is rare in port wine stain treatment. Most cases achieve significant lightening, making the mark much less noticeable. According to the Children’s Hospital of Philadelphia, maintenance treatments may be needed over the years to sustain results.
PHACE Syndrome: The Scary Acronym You Might Not Need to Worry About
PHACE syndrome affects some babies with large facial hemangiomas. The acronym stands for Posterior fossa brain malformations, Hemangioma, Arterial anomalies, Cardiac defects, and Eye abnormalities. It sounds terrifying, but most cases are manageable with proper monitoring.
Large facial hemangiomas, bigger than 5 cm, require screening. Lesions covering multiple facial areas also need evaluation. Testing is required before starting propranolol medication to ensure safety. The workup includes brain MRI, heart ultrasound, eye exam, and arterial MR imaging.
This seems like overkill, but it catches serious issues early before complications develop.
Certain arterial malformations increase stroke risk with beta-blocker therapy, making screening essential. Brain abnormalities detected may need monitoring but rarely require treatment. Heart defects might require cardiology follow-up and ongoing care. Early detection prevents complications and guides treatment decisions.
Most children with PHACE syndrome develop normally with proper management from a multidisciplinary team. The screening is more common than the serious problems it finds. Think of it as thorough safety checking rather than assuming something’s wrong with your child.
According to Children’s Hospital Boston, a comprehensive evaluation allows physicians to coordinate care effectively and prevent potential complications.
Making the Treatment Decision: When to Treat vs. When to Wait
Not every vascular lesion needs treatment right away. Sometimes the best approach is watchful waiting with periodic monitoring. But how do you decide? The answer depends on location, growth pattern, potential complications, and your family’s concerns about appearance or function.
Reasons to Treat Now:
- Functional Problems: Lesions blocking vision, affecting breathing, or interfering with feeding require immediate intervention
- Rapid Dangerous Growth: Expansion near vital structures with potential for complications needs prompt treatment
- Ulceration: Open wounds causing pain, bleeding, or infection risk benefit from medical therapy
- Psychosocial Impact: Large facial lesions affecting your family’s quality of life may warrant early treatment
- Prevention Strategy: Treating early can prevent worse problems later, particularly with port wine stains
Reasons to Watch and Wait:
- Small, Uncomplicated Lesions: Those not affecting function or located in safe areas can be monitored
- Already Shrinking: Hemangiomas past the growth phase and involuting well may not need intervention
- Medical Reasons: Children with conditions that make treatment risky may benefit from observation
- Personal Choice: Your family’s preference matters after understanding all risks and benefits
Some lesions treated early could have resolved fine without intervention. Some lesions watched carefully end up needing treatment later anyway. No crystal ball exists to predict every case perfectly. Experienced pediatric specialists use research data and clinical experience to guide recommendations. Your family’s concerns and values matter in the decision, and second opinions are reasonable for complex vascular anomalies.
Conclusion: Most Vascular Lesions Have Happy Endings
Take a breath—most childhood vascular lesions are manageable conditions with excellent outcomes. Whether you’re dealing with an infantile hemangioma that fades naturally or a vascular malformation treated successfully with laser surgery, modern medicine offers excellent options. The vast majority of children with these conditions grow up healthy and happy, participating fully in normal activities without restrictions.
Getting a proper diagnosis from experienced pediatric specialists provides the foundation for good care. Understanding which category your child’s lesion falls into helps you know what to expect. Knowing the warning signs that require immediate attention gives you confidence in when to seek urgent care versus routine follow-up.
Schedule a consultation at Millcreek Dermatology for expert evaluation of your child’s vascular lesion and personalized treatment planning tailored to your family’s needs.
FAQs
What is a vascular lesion?
A vascular lesion is an abnormality involving blood vessels or lymph vessels that can appear anywhere on the body. These fall into two main categories based on the ISSVA 2018 classification system: vascular tumors (such as infantile hemangiomas) that involve abnormal cell growth, and vascular malformations (such as port wine stains) that represent structural abnormalities present from birth. Vascular lesions can range from small cosmetic marks to larger lesions affecting function. Most are benign lesions that don’t pose serious health risks but may require treatment depending on their location and characteristics.
Are vascular lesions dangerous?
Most vascular lesions are not dangerous and represent benign conditions that don’t threaten your child’s overall health. However, certain situations require prompt medical attention. Lesions near vital structures like the airway or eyes can cause functional problems if left untreated. Rapidly growing hemangiomas may need beta-blocker therapy to prevent complications. Some children with large facial hemangiomas require screening for PHACE syndrome, which can involve internal abnormalities needing specialized care. Rare complications such as the Kasabach-Merritt phenomenon are medical emergencies requiring immediate intervention.
At what age do hemangiomas stop growing?
Most infantile hemangiomas complete their rapid growth phase by 12 months of age, though some continue expanding until 18-24 months. The proliferative phase typically peaks between 3 and 4 months of age, which is why early treatment often starts during this window. After growth stops, the plateau phase begins, followed by gradual involution over several years.
Should I avoid sun exposure on my child’s vascular lesion?
Protecting vascular lesions from sun exposure is important, as UV damage can worsen discoloration and reduce the effectiveness of future laser treatment for port-wine stains. Use baby-safe sunscreen with SPF 30 or higher, protective clothing, and shade when possible. Sun protection is especially important after laser treatments when the skin is more sensitive.
Can my baby with a hemangioma go swimming?
Yes, babies with hemangiomas can swim safely, though you should apply sunscreen to the lesion and surrounding skin to prevent sunburn. Ulcerated hemangiomas should be kept clean and dry until healed, so swimming may need to be avoided during that time. Children taking propranolol can swim, but always ensure proper supervision as with any infant in water.


