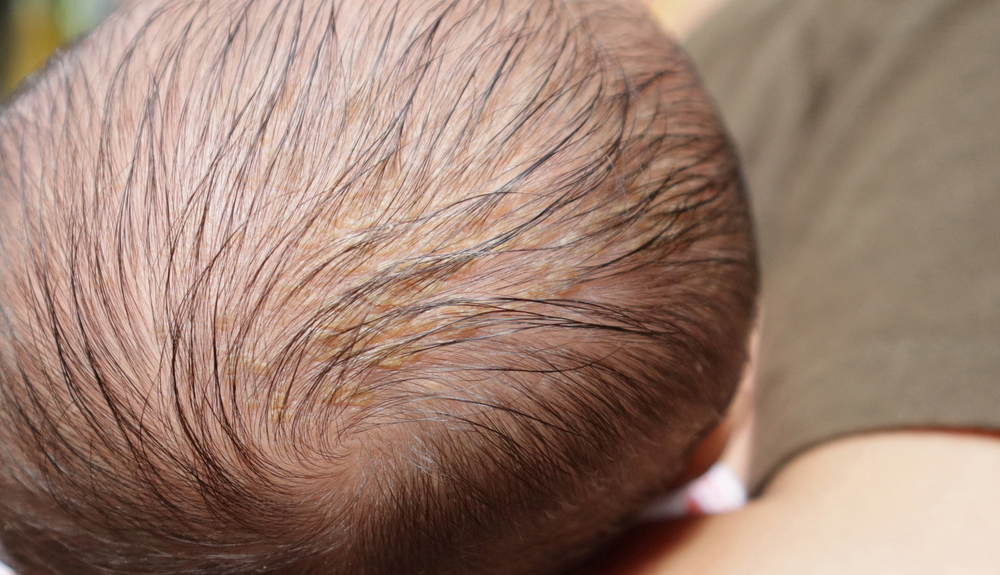
If you’ve noticed yellow, scaly patches on your baby’s scalp, you’re dealing with cradle cap—and yes, the shampoo you’re using could absolutely be making it worse. Many parents unknowingly choose products with harsh ingredients that strip natural oils from their baby’s scalp, triggering a vicious cycle of increased sebum production and more severe scaling.
Cradle cap affects up to 70% of infants, making it one of the most common skin conditions in early childhood. While generally harmless and self-resolving, using an inappropriate baby shampoo can prolong symptoms, increase discomfort, and even lead to secondary complications such as bacterial infections.
This guide reveals which ingredients can sabotage your baby’s delicate skin, the evidence-based treatment methods dermatologists recommend, and when professional care becomes necessary to manage infant seborrheic dermatitis effectively.
Overview: How to Stop Feeling Helpless About Your Baby’s Skin Condition
- Ingredient awareness matters: Sulfates, fragrances, and harsh chemicals in baby shampoo disrupt the scalp’s natural balance and worsen yellow scales.
- Gentle daily care works best: Oil pre-treatment combined with mild cleansing and soft brushing resolves most cases within weeks.
- Not all cradle cap needs medication: Conservative home treatment successfully manages the majority of cases without prescription products.
- Warning signs require action: Infection indicators, extensive spread, or persistent symptoms beyond 6-8 weeks warrant professional evaluation.
- Prevention prevents recurrence: Maintaining proper product selection and gentle routines keeps cradle cap from returning as your baby grows.
What exactly is cradle cap and why should you care?
Cradle cap is the common name for infantile seborrheic dermatitis, a skin condition characterized by greasy, yellow scales and crusty patches on the baby’s scalp. Unlike atopic eczema or other inflammatory conditions, cradle cap typically doesn’t cause itching or significant discomfort.
The condition results from a combination of factors working together on your baby’s delicate skin.
The Essential Facts Parents Need to Know
Understanding the basics helps you recognize and respond appropriately to this common newborn condition:
- Who it affects: Approximately 70% of infants develop cradle cap, typically within the first three months of life, regardless of gender, ethnicity, or feeding method
- What it looks like: Yellow, greasy scales or thick crusty patches primarily on the scalp, caused by overactive sebaceous glands producing excess oil
- Where it appears: Mainly affects the scalp but can extend to eyebrows, behind ears, and occasionally the diaper area or other skin creases
- Why it happens: Overactive oil glands combined with naturally occurring yeast overgrowth on the skin surface, influenced by maternal hormones still present after birth
- When to expect it: Symptoms emerge between 2-6 weeks of age, peak around 3 months, and usually resolve naturally by 12 months
According to Johns Hopkins Medicine, the condition involves overproduction of sebum and proliferation of Malassezia yeast on the scalp.
How It Differs from Other Baby Skin Conditions
Cradle cap stands apart from similar-looking conditions in several key ways. Unlike atopic dermatitis or atopic eczema, seborrheic dermatitis rarely causes significant itching or discomfort for infants.
The greasy, yellow appearance distinguishes it from dry, red patches typical of eczema. It’s not a fungal infection or bacterial infection in its initial stages, though it can become secondarily infected if thick scales aren’t properly managed.
Are you accidentally making your baby’s cradle cap worse?
The wrong shampoo doesn’t just fail to help cradle cap—it actively makes the condition worse by disrupting your baby’s scalp natural protective barrier. Many well-meaning parents choose products that seem gentle but contain problematic ingredients.
Understanding which components cause harm helps you make informed choices during bath time.
The Shampoo Ingredients Sabotaging Your Baby’s Scalp
Certain common ingredients in baby care products can exacerbate seborrheic dermatitis rather than improve it. These chemicals work against your baby’s developing skin rather than supporting its natural healing processes.
Ingredients to AVOID completely:
- Sodium lauryl sulfate (SLS) and sodium laureth sulfate (SLES): These harsh surfactants create impressive foam but strip essential oils, causing the scalp to overproduce sebum in compensation
- Artificial fragrances and dyes: Complex chemical mixtures that trigger allergic reactions or contact dermatitis in sensitive infant skin
- Parabens (methylparaben, propylparaben, butylparaben): Preservatives that can cause inflammatory responses in babies with existing skin conditions
- Alcohol-based ingredients (ethanol, isopropyl alcohol): Drying agents that worsen scaling and trigger rebound oil production
- Adult anti-dandruff shampoo formulations: Too aggressive for infant skin and contain active ingredients not appropriate for babies
The mechanism behind this damage involves disruption of your baby’s scalp protective lipid barrier. When sulfates compromise this barrier, the skin becomes more susceptible to irritation and bacterial overgrowth.
Harsh shampoos create a destructive cycle: they strip natural oils, the scalp responds by producing excessive sebum, and the greasy scales become even more pronounced. The pH imbalance compounds the problem—adult shampoos typically have a pH between 6-8, while a baby’s scalp maintains a more acidic pH around 5.5.
Even products labeled “natural” can be problematic. Natural fragrances still contain complex compounds that may irritate delicate seborrheic glands and worsen yellow patches.
Color additives serve no functional purpose and represent unnecessary exposure to potential allergens during vulnerable developmental stages.
What to Look for Instead
Appropriate products prioritize gentleness over marketing appeal. Look for tear-free, fragrance-free formulas specifically designed for infant use.
Mild cleansing agents like coco-glucoside or decyl glucoside effectively cleanse without over-drying the baby’s scalp. Products explicitly labeled “sulfate-free” and “paraben-free” reduce exposure to problematic chemicals.
According to the National Eczema Association, gentle cleansers help maintain the skin barrier while managing seborrheic dermatitis symptoms.
The Treatment Method That Actually Works (According to Dermatologists)
Evidence-based treatment for cradle cap combines gentle mechanical removal with appropriate cleansing products. The goal isn’t to aggressively scrub away scales but to soften them gradually and support your baby’s natural healing process.
Most cases respond well to conservative home care when approached systematically.
The Debate: Minimal Intervention vs. Active Treatment
Two philosophical approaches dominate discussions of cradle cap management. The gentle care philosophy advocates minimal intervention, emphasizing that this self-limiting skin condition resolves naturally without aggressive treatment.
The active treatment approach recommends early intervention with medicated products to prevent bacterial infections that can develop when thick scales create environments where harmful bacteria, such as Staphylococcus aureus, proliferate.
Medical consensus supports a middle ground: gentle daily cleansing with appropriate products, reserving medicated shampoos for persistent cases that don’t respond to conservative care within 6-8 weeks.
The Step-by-Step Treatment Process That Works
This systematic approach has been refined through decades of dermatological practice and research on infant seborrheic dermatitis:
- Pre-treat with oil (15-30 minutes before bath): Apply mineral oil, petroleum jelly, or coconut oil to affected areas. Gently massage with clean fingertips in circular motions to soften adherent, crusty patches.
- Use lukewarm water and gentle shampoo: Wash daily during active flare-ups with mild, fragrance-free baby shampoo. Use fingertip circular motions around hair follicles—never aggressive scrubbing that could damage delicate skin.
- Soft-brush removal: After shampooing, use a soft-bristled brush, baby brush, or a clean soft toothbrush to remove loosened scales gently. Work systematically in small sections from front to back using light pressure.
- Pat dry gently: Use baby bath towels and pat the scalp rather than rubbing, which can cause irritation or water blisters.
Consistency matters more than intensity. Daily gentle care beats weekly aggressive treatment every time.
Baby oil, olive oil, or borage oil work well for pre-treatment, though mineral oil and petroleum jelly remain the most recommended options due to their purity and low allergenic potential. Some parents successfully use coconut oil, though it occasionally causes reactions in highly sensitive infants.
When Medicated Products Are Actually Necessary
Most cases of cradle cap resolve with gentle home care alone. However, persistent symptoms despite 4-6 weeks of consistent, appropriate treatment may require prescription interventions.
Dermatologists may prescribe a 2% ketoconazole shampoo, which has shown 70-80% efficacy in clinical studies for resistant infant seborrheic dermatitis. These medicated shampoos address the yeast overgrowth component without the harsh effects of traditional anti-dandruff formulations.
Mild hydrocortisone cream (0.5-1%) may be recommended for areas with significant inflammation, but only under medical supervision for limited periods. Prolonged use of topical steroids or corticosteroid cream on infant skin can cause thinning or other adverse effects.
Kids Health notes that most cases clear up within a few months with basic home treatment, though some babies need additional medical attention.
Red Flags: When Your Baby Needs a Dermatologist NOW
While cradle cap is generally benign, certain warning signs indicate complications requiring immediate professional evaluation. Recognizing these red flags prevents serious complications and ensures optimal outcomes.
Don’t wait if you notice any concerning changes beyond typical yellow scales and scaly patches.
Warning Signs You Shouldn’t Ignore
Certain symptoms indicate your baby needs evaluation by a healthcare professional rather than continued home care:
Seek professional care immediately if you notice:
- Signs of infection: Redness spreading beyond scaly rash areas, warmth when touching the scalp, pus or fluid discharge, foul odor, or fever accompanying skin symptoms
- Extensive spread: Seborrheic dermatitis symptoms appearing on face, neck, throughout the diaper area, or across the body rather than just the scalp
- Persistent symptoms: No improvement after 6-8 weeks of proper home treatment with appropriate products and techniques
- Severe presentation: Thick, adherent crusty patches covering large portions of the scalp from the initial onset
- Baby’s discomfort: Obvious pain when touching affected areas, excessive scratching at the scalp, or increased fussiness specifically during bath time
Don’t wait if you see signs of infection. Bacterial complications can escalate quickly in infants with compromised skin barriers.
Secondary bacterial infection represents the most serious complication. When thick scales create environments where harmful bacteria proliferate, you may notice increased redness, warmth, and sometimes pustules forming around affected areas.
These infection symptoms require immediate medical attention and typically necessitate prescription antibiotic treatment.
What Professional Care Provides
A medical doctor specializing in pediatric dermatology can provide a comprehensive evaluation that is not available through home assessment. A physical exam by qualified professionals helps distinguish cradle cap from conditions such as atopic dermatitis, psoriasis, or fungal infections that mimic seborrheic dermatitis but require different approaches.
Dermatologists can prescribe prescription-strength antifungal treatments, medicated creams, or appropriate topical steroids when conservative care fails. They also provide valuable reassurance for anxious parents dealing with persistent skin conditions.
Prevention Strategies to Keep Cradle Cap from Coming Back
Preventing recurrence requires maintaining healthy scalp care routines even after symptoms have completely cleared. Some babies experience intermittent flare-ups during teething, illness, or growth spurts.
Understanding prevention strategies helps you respond quickly at the first signs of returning scales.
Building a Healthy Scalp Routine
Consistent, gentle care practices maintain the scalp’s natural balance and prevent the buildup of dead skin cells that contribute to scaling.
Daily maintenance habits:
- Continue gentle, daily shampooing even after yellow patches resolve to prevent buildup of oils and skin flakes
- Use only fragrance-free products specifically formulated for infant use, avoiding harsh shampoos marketed for adults
- Maintain appropriate humidity in your baby’s room to prevent excessive drying that triggers compensatory oil production
- Regular soft-bristle brushing during bath time prevents scale accumulation before it becomes problematic
- Wash bedding and clothes in gentle, fragrance-free detergent to minimize additional irritation from environmental sources
Some babies show patterns of flare-ups in response to specific triggers, such as seasonal changes or developmental phases. Return to the oil pre-treatment routine at the first signs of returning scales rather than waiting for severe symptoms.
According to the National Center for Biotechnology Information, maintaining gentle cleansing routines helps prevent recurrence of seborrheic dermatitis.
What NOT to Do
Certain common mistakes can undo your prevention efforts or trigger new flare-ups. Never pick or scratch scales aggressively—this damages the skin barrier and can introduce bacterial infections.
Don’t skip washing thinking it will “preserve oils.” Regular gentle cleansing actually helps maintain healthy balance better than infrequent washing.
Avoid layering multiple products, such as baby lotion or barrier cream, heavily on affected areas, as they can trap oils and dead skin cells.
Conclusion
The shampoo you choose significantly impacts your baby’s cradle cap trajectory. Harsh ingredients containing sulfates, fragrances, or inappropriate pH levels create a vicious cycle of irritation and increased sebum production that prolongs this common skin condition.
The good news? Most cases resolve completely with gentle, consistent care using appropriate products and techniques.
Concerned about your baby’s cradle cap symptoms? Schedule an appointment with Millcreek Dermatology for expert evaluation and comprehensive treatment planning.
FAQs
What is cradle cap?
Cradle cap is the common name for infantile seborrheic dermatitis, a skin condition that causes yellow, greasy scales or crusty patches on a baby’s scalp. It results from overactive oil glands that produce excess sebum, combined with naturally occurring yeast on the skin. The condition typically appears within the first few months of life and affects up to 70% of infants. Despite its appearance, cradle cap is generally harmless, doesn’t usually cause itching, and typically resolves on its own by 12 months of age with gentle home care.
How to get rid of cradle cap?
The most effective approach combines gentle daily treatment with appropriate products. Start by applying mineral oil, petroleum jelly, or baby oil to the affected areas 15-30 minutes before bath time to soften the scales. During the bath, use a mild, fragrance-free baby shampoo with lukewarm water and gentle circular motions. After shampooing, use a soft-bristled brush to remove loosened scales gently. Pat the scalp dry with a soft towel. Consistency matters—daily gentle care typically shows improvement within 2-4 weeks. If symptoms persist beyond 6-8 weeks, consult a dermatologist about medicated shampoos containing ketoconazole.
Why do babies get cradle cap?
Babies develop cradle cap due to a combination of factors related to their developing skin. Overactive sebaceous glands produce excess oil on the scalp, influenced by maternal hormones that remain in the baby’s system after birth. This excess oil creates an environment in which the naturally occurring Malassezia yeast proliferates on the skin surface. The baby’s developing immune system is still learning to regulate the balance of microorganisms on their skin, making them more susceptible to this overgrowth. Unlike bacterial or fungal infections, cradle cap involves an imbalance of normal skin flora rather than harmful pathogens.
Does cradle cap stop hair growth?
Cradle cap does not permanently affect hair growth or cause lasting hair loss. While thick scales may temporarily make hair appear thinner or cause some hair to come out when scales are removed, this is normal shedding. The hair follicles beneath the scales remain healthy and undamaged. Once the cradle cap resolves, hair growth continues normally without any long-term effects. If you notice significant hair loss, bald patches that persist after scales clear, or other concerning symptoms, consult a pediatric dermatologist to rule out other conditions unrelated to typical seborrheic dermatitis.
How to treat dry scalp on toddler?
Treating dry scalp in toddlers requires gentle approaches similar to those used for cradle cap, but adjusted for older children. Use a mild, moisturizing shampoo specifically formulated for sensitive skin, washing 2-3 times per week rather than daily to avoid stripping natural oils. Apply a small amount of coconut oil or mineral oil to the scalp after bathing to maintain moisture. Ensure adequate hydration and humidity in your home, especially during dry winter months. Avoid harsh shampoos containing sulfates or fragrances. If dryness persists, appears severe, or is accompanied by redness or irritation, schedule an evaluation with a dermatologist to determine whether the condition requires specialized treatment beyond basic dry-skin care.


